What Is Retinal Detachment?
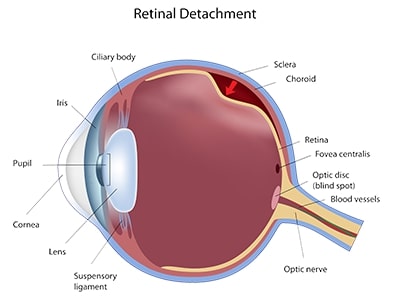
When your retina, the thin layer of tissue at the back of the eye, pulls away from its normal position, this is retinal detachment. Because the detachment separates the retinal cells from the layer of blood vessels that provides oxygen and nourishment, this is an emergency situation to prevent vision loss.

There are three different types of retinal detachment: rhegmatogenous, tractional, and exudative detachment. Each requires surgery to save the patient’s vision.
The sudden appearance of floaters and flashes in your vision are the most common warning signs that your retina is beginning to detach.
The Causes Of Retinal Detachment
The different forms of retinal detachment have different causes:
- Rhegmatogenous — This is the most common form of retinal detachment. Detachment is caused by a hole or tear in the retina that allows fluid to pass through and collect underneath the retina, pulling the retina away from the underlying tissues.
Rhegmatogenous detachment is usually caused by normal aging. As we age, the gel-like material that fills the inside of the eye, the vitreous, can change in consistency and shrink or become more liquid. This separation usually happens without incident, but one complication is a tear. As the vitreous separates or peels off the retina, it may tug on the retina with enough force to create a retinal tear. If not addressed, the liquid vitreous can pass through the tear into the space behind the retina, causing the retina to detach.
- Tractional — In people with poorly controlled diabetes and other conditions, scar tissue can grow on the surface of the retina. This scar tissue can cause the retina to pull away from the back of the eye.
- Exudative — In this type of detachment, fluid accumulates beneath the retina, but there aren’t any holes or tears in the retina. Exudative detachment can be caused by age-related macular degeneration, injury to the eye, tumors, or inflammatory disorders.
Retinal Detachment Symptoms
Symptoms of retinal detachment include the development of floaters and flashes. Bleeding from the tear in the retina will cause floaters, which can come in a variety of shapes. The pulling of the vitreous (the jelly inside the eye that shrinks as we age) will cause the flashes. As the retina detaches images at the edge of one’s vision will become blurry.
Who Is A Good Candidate For Boston Retinal Detachment Treatment?
Patients experiencing any of the symptoms associated with retinal detachment, including floaters, flashes, and blurred or darkened vision, should contact North Suburban Eye Associates, P.C. to schedule an examination in the greater Boston area.
Is Retinal Detachment Painful?
Retinal detachment doesn’t involve any pain, but you’ll likely see warning signs before it occurs or has advanced. These are discussed in the symptoms section, but they include the sudden appearance of many floaters in your vision field. Flashes are also likely. Your vision may blur, and your peripheral vision may start to diminish.
How A Detached Retina Is Treated
At North Suburban Eye Associates, two of our board-certified ophthalmologists, Dr. Desai and Dr. Witkin, specialize in surgery to repair retinal detachment. Surgery is almost always necessary to repair a retinal tear, hole, or full detachment.
If the retina has a tear or hole, but has not detached, Dr. Desai or Dr. Witkin may perform two procedures: photocoagulation or cryopexy. Photocoagulation uses a laser beam directed into the eye through the pupil. The laser energy burns around the retinal tear, creating scarring that attaches the retina to the underlying tissue. Cryopexy uses a freezing probe applied to the outer surface of the eye directly over the tear. The freezing creates scar tissue that helps secure the retina to the eye wall.
If you have a detached retina, you’ll need surgery soon after your diagnosis. Here are three methods we may employ:
- Pneumatic retinopexy — In this surgery, Dr. Desai or Dr. Witkin injects a bubble of air or gas into the center of your eye, the vitreous cavity. The bubble then pushes the area of the retina containing the hole or holes back against the outer wall of the eye. This stops the flow of fluid into the space behind the retina. Cryopexy may then be used to repair a break in the retina. Fluid under the retina is absorbed and the retina can then adhere to the wall as it formerly did. Patients usually need to hold their head in a certain position to keep the gas bubble in the proper position; this may be required for a period of several days.
- Scleral buckling — In this method, a piece of silicone material is sutured to the white of your eye (the sclera) over the affected area. This procedure indents the wall of the eye and relieves some of the force caused by the vitreous tugging on the retina. If you have several holes or tears, we may place silicone around the entire eye, similar to a belt. This doesn’t affect vision and is usually placed permanently.
- Vitrectomy — In a vitrectomy, we remove the vitreous along with any tissue that is tugging on the retina. Air, gas, or silicone oil is then injected into the vitreous space to help flatten the retina back against the wall. Eventually, the air, gas, or liquid will be absorbed, and the vitreous space will refill with body fluid.
Can A Retinal Detachment heal on its own?
Your detached retina will not heal without intervention, and this isn’t something to mess around with. Time you wait to receive treatment from our experienced team at North Suburban Eye Associates simply increases your vision loss. These are emergency situations.
Recovery Time You Should Expect After Treatment
Your recovery depends upon the method of surgery used. Each of the three procedures for a detached retina have different timelines, but the overall range for recovery is from two to six weeks.
- For pneumatic retinopexy, the recovery time is approximately three weeks. The most difficult part of this recovery is the need to maintain a specific head position for several days to keep the bubble in place long enough to repair the detachment.
- For scleral buckling, it is approximately two to four weeks. You’ll need antibiotic eyedrops to reduce the risk of infection, and you’ll likely wear an eye patch for a short period of time.
- For vitrectomy, recovery time is approximately four to six weeks. These procedures have the least involved recovery from a standpoint of what you need to do.
During your consultation, one of our doctors we will discuss your recovery in detail.
Patient Testimonial
"I highly recommend North Suburban Eye Associates. The entire staff works as a team to ensure a pleasant and comfortable visit. I would, without hesitation, trust my eye care and needs to NSEA."
What Happens If Retinal Detachment Is Left Untreated?
If the retinal detachment has affected the vision in the center of the eye, it is likely that even with surgery, this vision will not be restored. For this reason, it is important to seek immediate care if you believe you might be suffering from retinal detachment.

When You Can Return To Normal Activities
Expect at least 4 to 6 weeks for most normal activities, although there can be wide variation with the patient. The key is to avoid increasing blood pressure to the face and eyes through strenuous exercise or activity or heavy lifting. Dr. Shilpa Desai or Dr. Andre Witkin will clear you for activities as they follow your recovery.
Schedule A Boston Retinal Detachment Consultation
If you suffer from any symptoms of retinal detachment, contact North Suburban Eye Associates, P.C. today at 781-245-5200 to schedule a consultation. Our practice serves Wakefield, Winchester, and the surrounding Boston area.
