What Is Diabetic Retinopathy?
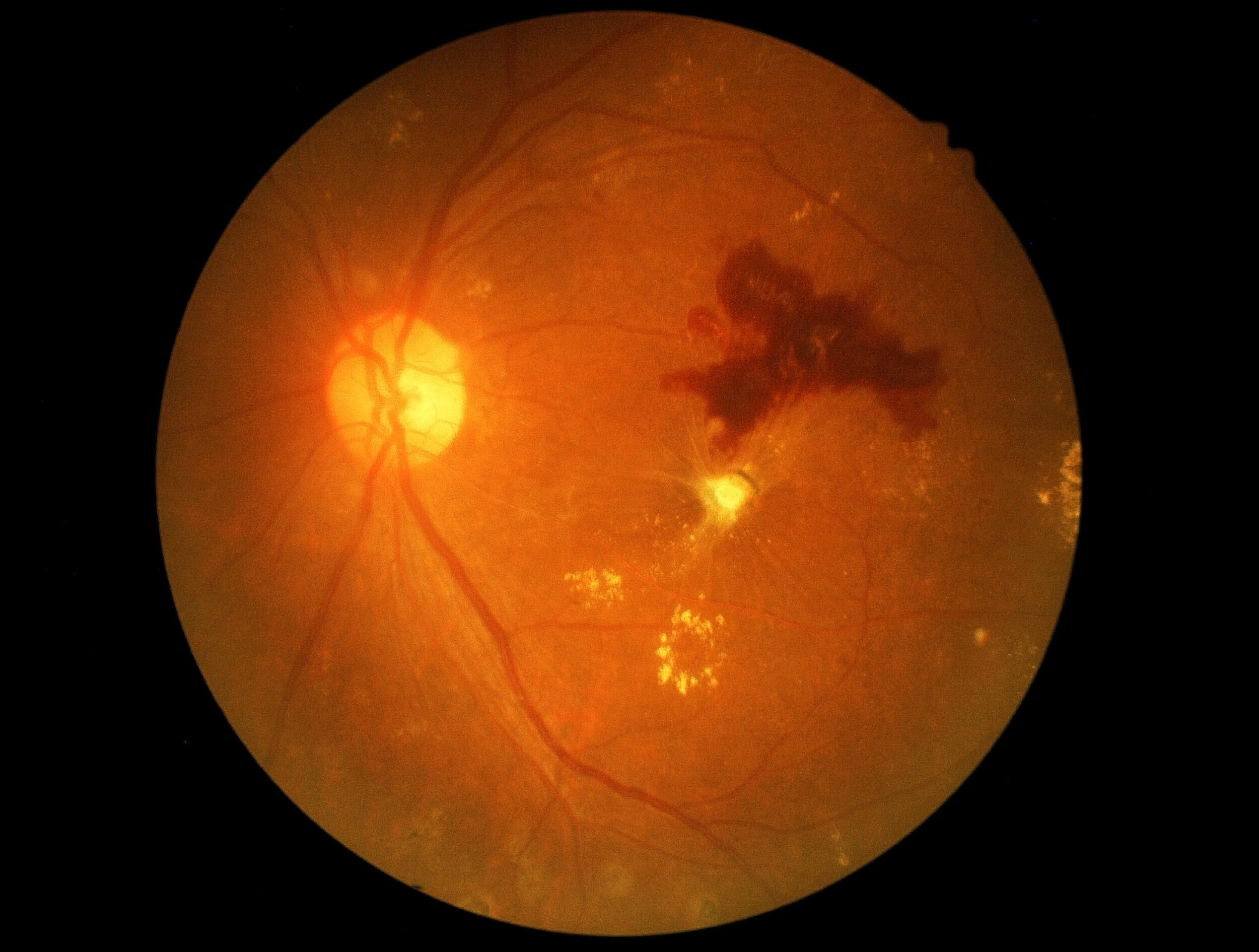
What Are The Types Of Diabetic Retinopathy And What’s The Difference?
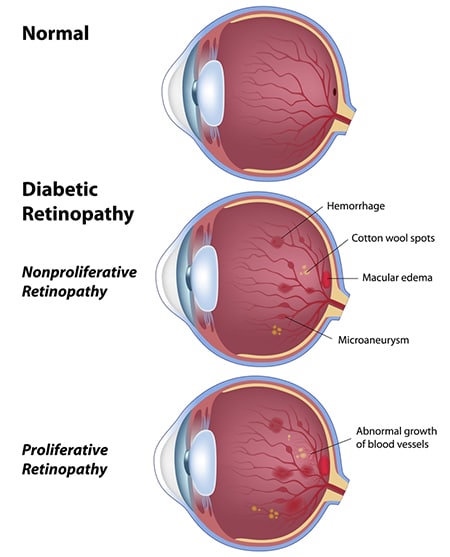
There are two types of diabetic retinopathy:
Nonproliferative Diabetic Retinopathy
This is the more common form. New blood vessels aren’t growing. Instead, the walls of the blood vessels in the retina weaken. Smaller vessels may develop bulges that can leak blood and other fluid into the retina. Larger vessels can become irregular in diameter. This early form of diabetic retinopathy can progress to the advanced form as more blood vessels become blocked.
Proliferative Diabetic Retinopathy
In this more severe form of retinopathy, damaged blood vessels close off, instigating the growth of new, abnormal blood vessels in the retina. These can leak into the vitreous, the jelly-like filling of the center of the eye. Scar tissue will often form due to the new blood vessel growth, and this can cause the retina to detach from the back of the eye.
The abnormal blood vessels may also interfere with the flow of fluid out of the eye, increasing pressure in the eyeball. This is glaucoma and the increased pressure can damage the optic nerve.
What Are The Symptoms Of Diabetic Retinopathy?
Patients with diabetic retinopathy may not experience any changes in vision, so it is important for those with diabetes to have regular eye exams. North Suburban Eye Associates provides eye examinations at all 3 of our locations in the greater Boston area.
The most common symptoms experienced are: blurred vision, sudden and severe loss in vision, rings around lights, dark spots, or flashing lights. If you notice any of these symptoms call North Suburban Eye Associates to schedule an appointment.
What Are The Four Stages Of Diabetic Retinopathy?
1. Mild Nonproliferative Retinopathy
At this stage, microaneurysms occur. They are small areas of balloon-like swelling in the retina’s tiny blood vessels. These do not affect vision and often go unnoticed.
2. Moderate Nonproliferative Retinopathy
Now the blood vessels that nourish the retina are blocked. This will often cause visible changes in the retina.
3. Severe Nonproliferative Retinopathy
In this stage, many more blood vessels are blocked, depriving several areas of the retina of their blood supply. These areas of the retina send signals to the body to grow new blood vessels for nourishment.
4. Proliferative Retinopathy
The most advanced stage. Now, as the retina sends signals that it needs nourishment, new blood vessels are created, but they are abnormal and fragile. They grow along the retina and along the surface of the clear, vitreous gel that fills the inside of the eye. The vessels aren’t the problem, as alone they don’t cause any symptoms or vision loss. The problem is their thin, fragile walls. These leak blood and can lead to severe vision loss and even blindness.
Diabetic Retinopathy Treatment
For slight cases of diabetic retinopathy, treatment may not be necessary, but close monitoring for changes and progression is important. In more advanced cases laser photocoagulation may be performed.
During this surgery, our surgeons use a laser to generate a quick burst of light energy to treat the leaking blood vessels and reduce the abnormal blood vessels to prevent further bleeding and scarring. If the bleeding is severe a Vitrectomy may need to be performed to remove the blood from the center of the eye. Since diabetes continuously affects the body, these treatments will not cure diabetic retinopathy.
What Is Recovery Like After These Treatments?
With laser treatments, you may have some discomfort and your vision may be blurry for a day or two, but most patients can return to normal activities immediately after these treatments. Some patients experience flashes of light at night or when looking at anything with a white background. These issues will decrease and resolve.
With injections, your visual acuity will also be impacted, but will significantly improve within a week or two. Recovery varies between the different drugs injected.
Vitrectomy requires the most involved recovery, with full recovery taking between 4 to 6 weeks. Some patients may be required to lay face down for a period of time to help their eye heal properly. Typical activities such as driving, reading, and exercise will need to wait for at least a week, maybe more.
What Are The Risk Factors For Developing Diabetic Retinopathy?
If you have diabetes, you can develop diabetic retinopathy. These factors increase your risk:
- Longer duration having diabetes
- Poor control of your blood sugar levels
- High cholesterol
- High blood pressure
- Pregnancy
- Tobacco use
- Being African American, Hispanic, or Native American

Will my Diabetic Retinopathy Require Continued Treatment?
Diabetes continues to affect the body, so a patient's diabetic retinopathy isn't fully cured. Patient's will still need to see their ophthalmologist for annual eye exams so they can keep an eye out for the development of abnormal blood vessels or possible blood leakage.
After having one of the possible treatments, such as focal or scatter laser treatment or a vitrectomy, you shouldn't think you can forget about your diabetic retinopathy. You'll need to remain vigilant to prevent further issues or vision loss.
What Issues Can Diabetic Retinopathy Cause If Left Untreated?
These abnormal blood vessels may either bleed or leak fluid or grow on the surface of the retina causing bleeding and scarring. Both of these complications can result in permanent loss of vision.
Diabetic Retinopathy FAQs
How often should I get screened for diabetic retinopathy if I have diabetes?
Most patients with diabetes should receive a comprehensive dilated eye exam at least once a year. Patients with type 1 diabetes are typically advised to begin screening within five years of diagnosis, while those with type 2 diabetes should be screened as soon as they are diagnosed. If diabetic retinopathy is detected, your eye doctor may recommend more frequent visits to closely monitor the retina and begin treatment if needed. Regular screening allows specialists to detect changes in the retina before vision symptoms develop.
How is diabetic retinopathy diagnosed?
Diagnosing diabetic retinopathy involves a detailed examination of the retina using specialized imaging technology. During a comprehensive eye exam, the ophthalmologist will dilate the pupils to examine the retina and optic nerve more clearly. Additional tests may include optical coherence tomography (OCT), which produces detailed cross-section images of the retina, and fluorescein angiography, a diagnostic test that highlights leaking or abnormal blood vessels. These imaging tools allow doctors to identify early retinal changes and determine the stage of disease progression.
Is diabetic retinopathy reversible with early treatment?
In many cases, early-stage diabetic retinopathy can be stabilized and prevented from progressing when detected early. While treatments cannot always reverse existing retinal damage, prompt care can significantly reduce the risk of severe vision loss. Laser therapy, injections, and surgical procedures help control abnormal blood vessels and retinal swelling. Consistent medical monitoring and diabetes management also play an important role in protecting vision.
Are there lifestyle changes that can help slow the progression of diabetic retinopathy?
Yes. Managing overall health is a key part of slowing the progression of diabetic eye disease. Maintaining stable blood sugar levels, controlling blood pressure and cholesterol, and following a healthy diet all help protect the delicate blood vessels of the retina. Regular exercise, avoiding tobacco, and attending routine eye exams are also important steps. These habits work together with medical treatments to reduce the likelihood of further retinal damage.
What is the long-term outlook for vision after treatment?
The prognosis for diabetic retinopathy varies depending on how early the disease is detected and treated. Many patients maintain functional vision for years when the condition is diagnosed early and carefully managed. Ongoing monitoring is essential because diabetes continues to affect blood vessels throughout the body, including those in the eye. With regular exams and proper treatment, ophthalmologists can often prevent severe vision loss and preserve visual function.
How is diabetic retinopathy different from age-related macular degeneration?
Diabetic retinopathy and age-related macular degeneration (AMD) both affect the retina, but they develop for different reasons. Diabetic retinopathy is caused by damage to retinal blood vessels from prolonged high blood sugar levels. AMD, on the other hand, is primarily associated with aging and changes in the macula, the central portion of the retina responsible for detailed vision. While symptoms such as blurred vision may appear similar, the underlying causes and treatment approaches differ significantly.
